It’s finished!!
The rebuilding of the new practice that began on 8th April 2024, has now been completed. Please give us a call to book an osteopath appointment on 02082987122, we think you’ll like it.

Thanks to all of our loyal osteopathic patients for sticking with us during the difficult process.
They all agree that it’s a lovely environment to be treated in!!
We’re in the new building!!
We’re back in the extension and things are starting to really take shape, please look for the blue sign when you are coming for your appointment and ring the bell. Feel free to park in front of the entrance to the osteopaths.
The outside still needs some work, but the inside is finished and we think it looks great, we really hope you agree!!
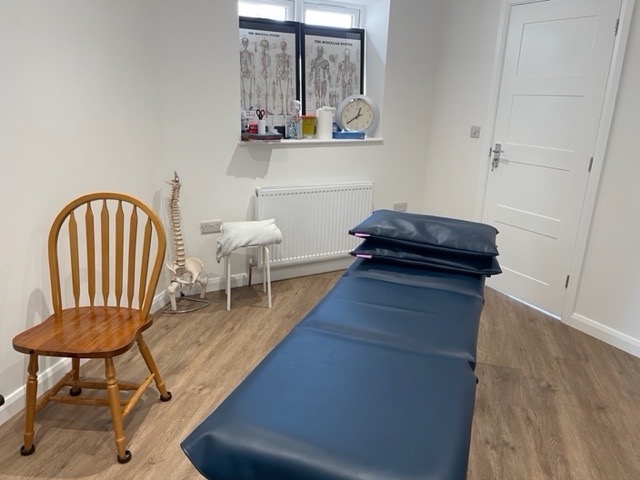
Build Update
Things are starting to take shape regarding the new osteopathic practice build. We are hoping the work will be completed within the next few weeks!

Until then we are still open at the Bexleyheath Osteopath Practice for appointments so give us a call on 02082987122 if you need to book. Our osteopaths look forward to seeing you soon!!
Temporary Relocation/Building Work
From Monday 8th April 2024 access will be gained to the Bexleyheath Osteopathic Practice via the front door of 4 Glengall Road as the building work commences on the new osteopath practice.
Please park in front of the house (instead of in front of the white garage door) and knock on the brown wooden door to gain access. Please try to park considerately as there should be space for 2 vehicles.

Whilst the new practice is being built, there is likely to be additional noise and inconvenience, but we will work hard with the builder to try to keep this to a minimum. We hope that the work will be completed by the Autumn, allowing us to improve the service and facilities we offer at the Bexleyheath Osteopathic Practice.
We apologise in advance for the inconvenience, and thank you for your patience!!
Update re building work
The Bexleyheath Osteopathic Practice is being rebuilt, but there has been a bit of a delay in the start date, so it’s currently business as usual. Please watch this space for any changes to our services… the car park and entrance are still in the same place for now, but will hopefully be changing in the coming weeks.
Give us a call if you need an osteopath, as our osteopaths are here for you.
The phone number is 02082987122.
We look forward to welcoming you to the Bexleyheath Osteopath Practice soon!!
Building work and Alix
Unfortunately, Alix has handed in her notice and is off to “pastures new”. She will be leaving the Bexleyheath Osteopathic Practice at the end of April 2024. Alix has worked as an osteopath at the practice for 4 years and we wish her well with any future osteopathic endeavours!!
Chris will probably work on his own whilst the practice is being redeveloped, and find a new osteopath to help him later in the summer.
Sorry for any inconvenience that the building work will cause, but we will remain open, and will have improved facilities when they are all complete!
Thank you for your ongoing custom.
Chris, Bexleyheath Osteopath
London School of Osteopathy
Chris is has just been offered a new job at The London School Of Osteopathy. He will now be teaching 3rd and 4th year students osteopathic manipulation as part of the osteopathy module. This appointment means he will not be available on Thursday’s during term time at the Bexleyheath Osteopathic Practice.
But don’t worry, Alix will be covering, so we can still offer you an appointment with an osteopath at a time that suits you.
Give us a call at Bexleyheath Osteopaths on 02082987122 if you need to book an appointment.
Latest Changes to our Coronavirus Policy
I am pleased to report that in keeping with recent changes to the Government advice in healthcare, it is no longer compulsory for patients or staff to wear masks as standard. We might, however, continue to wear masks for vulnerable patients.
Hopefully this is a sign that life is continuing to get back to normal, but if you are uncomfortable with this updated policy, and would like us to wear a mask when you visit, please just ask!!
I hope this news gives people confidence that we are continuing to adhere to all Government guidelines relating to Infection Prevention and Control (IPC)
At the Bexleyheath Osteopathic Practice we always want our patients to feel relaxed and safe, so call us now on 02082987122 if you want to book an appointment with one of our osteopaths.
We look forward to meeting you soon!
Just so you know...
We love helping people with osteopathic treatment, but are always realistic about what osteopathy can treat. It is for this reason that we only really treat musculoskeletal conditions at the Bexleyheath Osteopathic Practice.
Pain is a really complicated and unpredictable thing in humans, and whilst there is some quite good evidence supporting the techniques used by osteopaths, it is not always a “magic cure.”
Some patients need a short course of treatment, some however need longer courses, it is impossible to tell until we see you (..sorry!)
The path to becoming symptom free is not always uniform either and we warn all of our patients that there might be some "road bumps” along the way. We tend to ask people to gauge their condition "week on week", not necessarily "minute on minute” as pain levels often fluctuate depending on many factors.
We also warn patients that they might actually be sore immediately after treatment, as osteopathy can be quite challenging to the tissues that might be damaged. It is for this reason that we try to make people aware that they might even feel a little bit worse after undergoing osteopathic manipulation. This should be very short term and manageable, but it’s important to us that patients understand that it can happen.
It is actually quite easy to over treat some conditions, which can lead to increased pain, this is why a session is not “set in stone”. We tend to take about 45 minutes to see a new patient, and then work on about a half an hour list for returning patients. Working longer and harder does not necessarily give better outcomes… would you ask a dentist to continue drilling when they have completed the treatment you have come for?
Thanks for reading, as we feel having realistic expectations about your visit to the Bexleyheath Osteopahtic Practice will help us to help you more effectively.
If you would like to book an appointment to see one of our osteopaths in Bexleyheath please give us a call on 02082987122 to arrange a convenient time. We look forward to meeting you at the Bexleyheath Osteopathic Practice soon!!
Sprained Ankle
A sprained ankle is an injury that occurs when you roll, twist or turn your ankle in an awkward way. This can stretch or tear the tough bands of tissue (ligaments) that help hold your ankle bones together. Normally the pain will be on the outside of your ankle.
Ligaments help stabilize joints, preventing excessive movement. A sprained ankle occurs when the ligaments are forced beyond their normal range of motion. Most sprained ankles involve injuries to the ligaments on the outer side of the ankle. The most commonly strained ligament in the human body is called the anterior talo-fibular ligament (ATFL)
Treatment for a sprained ankle depends on the severity of the injury. Although self-care measures and over-the-counter pain medications may be all you need, an evaluation might be helpful to reveal how badly you've sprained your ankle and to determine the appropriate treatment and managemant.
Signs and symptoms of a sprained ankle vary depending on the severity of the injury. They may include:
- Pain, especially when you bear weight on the affected foot
- Tenderness when you touch the ankle
- Swelling
- Bruising
- Restricted range of motion
- Instability in the ankle
- Popping sensation or sound at the time of injury
Call us if you have pain and swelling in your ankle and you suspect a sprain. Self-care measures may be all you need, but talk to an osteopath to discuss whether you should have your ankle evaluated. If signs and symptoms are severe, you may have significant damage to a ligament or a broken bone in your ankle or lower leg.
The following tips can help you prevent a sprained ankle or a recurring sprain:
- Warm up before you exercise or play sports.
- Be careful when walking, running or working on an uneven surface.
- Use an ankle support brace or tape on a weak or previously injured ankle.
- Wear shoes that fit well and are made for your activity.
- Minimize wearing high-heeled shoes.
- Don't play sports or participate in activities for which you are not conditioned.
- Maintain good muscle strength and flexibility.
- Practice stability training, including balance exercises.
If you want to book an appointment give us a call at the Bexleyheath Osteopathic Practice on 02082987122. We look forward to hearing from you.